Pharmaceuticals: client demographics and treatment
On this page:
In 2021–22, pharmaceuticals were reported as a drug of concern (either principal or additional) in 10.0% of all treatment episodes (21,185 episodes) (Table Drg.87).
- Pharmaceuticals were the principal drug of concern in 5.0% of treatment episodes (10,400 episodes) (Table Drg.87). This proportion relative to all drugs of concern has declined from 7.2% in 2012–13 (11,100 episodes).
- In the 10 years to 2021–22, pharmaceuticals were generally more likely to be reported as an additional rather than principal drug of concern. However, in 2021–22 the proportion of episodes with pharmaceuticals as an additional drug of concern has declined to 5.1%, (Table Drg.87).
- The most common additional drugs of concern reported with pharmaceuticals were amphetamines (22% or 1,400 episodes), cannabis (21% or 1,300 episodes) and alcohol (15% or 920 episodes) (Figure DRUGS 1, Table Drg.88).
Classification of pharmaceutical drugs in the AODTS NMDS
Pharmaceuticals are drugs that are available from a pharmacy—over the counter or by prescription—including opioids (such as codeine and oxycodone) and benzodiazepines (such as diazepam). Some pharmaceutical drug use is for non-medical purposes (Department of Health 2017).
Pharmaceuticals are not listed as a broad drug group in the Australian Standard Classification of Drugs of Concern (ASCDC) classification. In the AODTS NMDS report, the ‘pharmaceuticals’ drug classification includes the following 10 drug types: codeine, morphine, buprenorphine, oxycodone, methadone, benzodiazepines, steroids, other opioids, other analgesics, and other sedatives and hypnotics. Refer to the Technical notes and Key terminology and glossary for more information.
For information on pharmaceutical drug use and harms, please see:
Tobacco, alcohol and other drugs in Australia: Pharmaceuticals
National Drug Strategy Household Survey 2019 (Chapter 5: Non-medical use of pharmaceuticals)
Pharmaceuticals by drug type
In 2021–22, opioids and benzodiazepines accounted for 3 in 4 episodes provided for a pharmaceutical drug as the PDOC (76% or 7,934 episodes) (Table Drg.87). ‘Opioids’ includes codeine, morphine, buprenorphine, oxycodone, methadone and other opioids.
- Opioids as a group were a principal drug of concern in 2.2% of all treatment episodes and an additional drug of concern in 1.3% (4,700 and 2,600 episodes, respectively). Buprenorphine (1,400 episodes), methadone (950) and oxycodone (740) were the most common principal drug types recorded in opioid-related treatment episodes.
- Benzodiazepine was a principal drug of concern in 1.5% of treatment episodes and an additional drug of concern in 2.3% (3,200 and 4,800 episodes, respectively).
Over the 10 years to 2021–22:
- The number of treatment episodes with pharmaceuticals as the principal drug of concern decreased slightly, from 11,100 to 10,500 episodes. Relative to all other principal drugs of concern, the proportion of episodes for pharmaceuticals fell from 7.2% to 5.0%.
- The number of treatment episodes for benzodiazepines initially decreased from 2,400 episodes from 2012–13 to 1,700 episodes in 2015–16, increasing to 3,200 in 2021–22.
- The number of episodes for opioids peaked at 7,700 in 2013–14 before falling to 4,700 episodes in 2021–22 but fluctuated over time by drug type (Figure PHARMS 1; Table Drg.87).
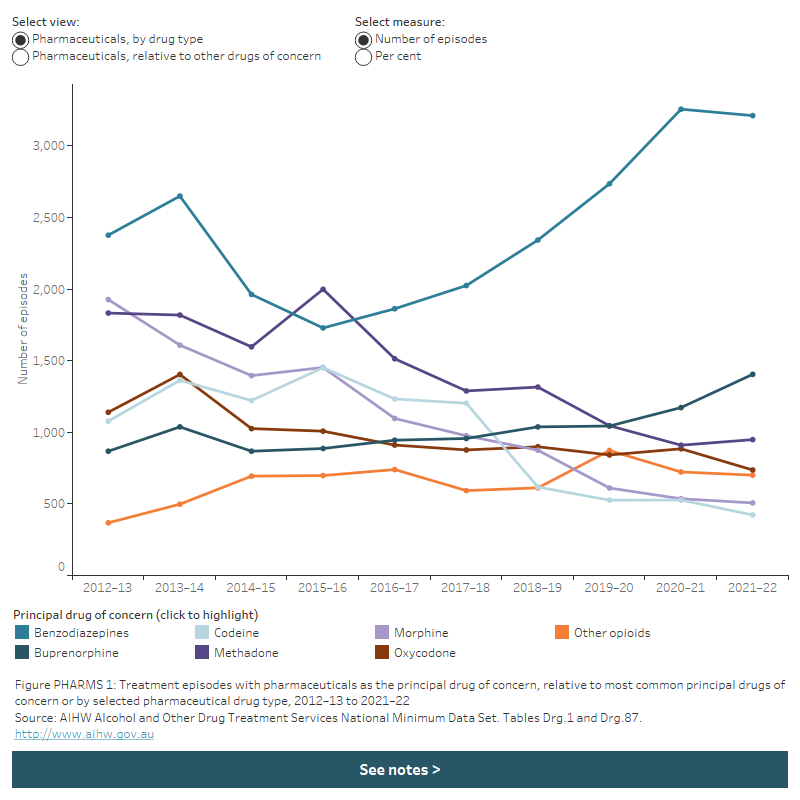
Figure PHARMS 1: Treatment episodes with pharmaceuticals as the principal drug of concern, by selected principal drugs of concern, 2012–13 to 2021–22
The line graph shows that amongst pharmaceutical drugs, benzodiazepines were the most common principal drug of concern for most years in the 10-year period to 2021-22, increasing from 2,377 episodes in 2012-13 to 3,212 episodes in 2021-22.
Filters allow the user to toggle between viewing episode data on pharmaceutical drugs by pharmaceutical drug type, or in relation to the 5 most common principal drugs of concern in the AODTS NMDS. Filters also allow the user to toggle between the number and proportion of episodes.
Client demographics
In 2021–22, around 6,155 clients received treatment for any pharmaceutical drug as the principal drug of concern (Table SC.30). Of these clients:
- 3 in 5 were male (61% of clients). The proportion of male clients ranged from 42% for codeine to 88% for steroids (Table SC.30).
- Over 1 in 2 were aged either 20–29 (25% of clients) or 30–39 (29%). The proportion of clients in each age group varied by PDOC:
- Clients receiving treatment for benzodiazepines had the highest proportion of people aged 10–19 (19% of clients).
- Most clients receiving treatment for opioids were aged either 30–39 or 40–49, ranging from 52% for oxycodone to 64% for buprenorphine (Table SC.31).
- Around 1 in 7 were Indigenous Australians (15% of clients). The proportion of Indigenous clients was highest for buprenorphine (29% of clients) (Table SC.32).
Treatment
In 2021–22, around 10,445 treatment episodes were provided to clients for pharmaceuticals as the principal drug of concern (Table Drg.87).
- The most common sources of referral were self/family (40% of episodes) and health services (39%). This was relatively consistent across drug types, but diversion was the most common referral source for steroid-related treatment episodes (33% of episodes) (Table Drg.90).
- The most common main treatment types were assessment only (30% of episodes) and counselling (22%) (Figure PHARMS 3; Table Drg.89).
- Most episodes took place in non-residential treatment facilities (74% of episodes); this was the most common treatment setting across drug types (Figure PHARMS 3; Table Drg.92).
- Three in 5 treatment episodes ended with a planned completion (60% of episodes; ranging from 49% for morphine as the PDOC to 76% for steroids). Just under 1 in 5 episodes ended unexpectedly (19%) (Figure PHARMS 2; Table Drg.91).
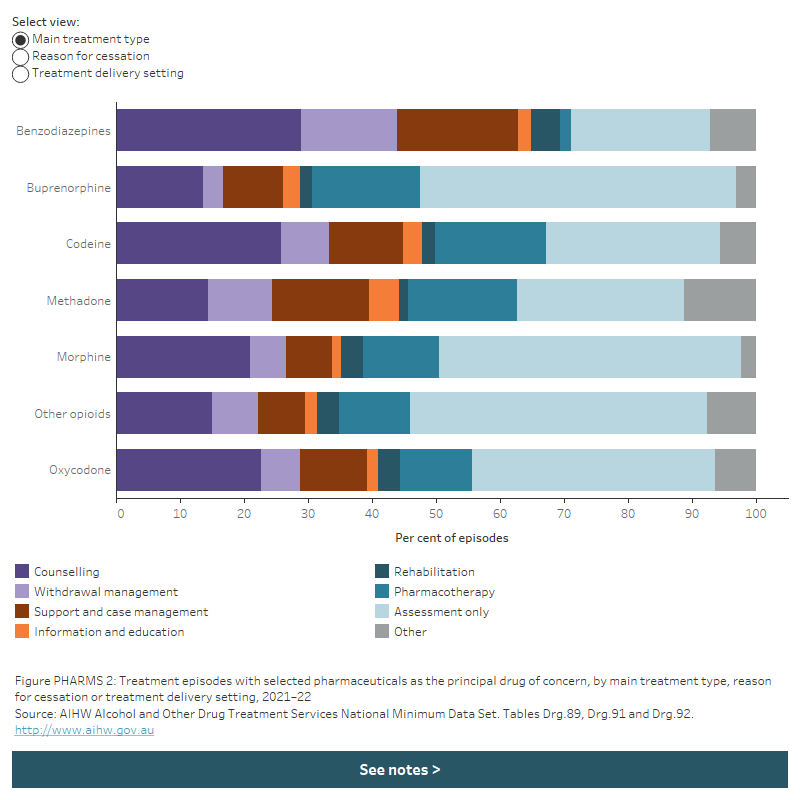
Figure PHARMS 2: Treatment episodes with selected pharmaceutical drugs as the principal drug of concern, by main treatment type, treatment delivery setting or reason for cessation, 2021–22
The stacked horizontal bar chart shows that in 2021–22 assessment only was the most common main treatment type among most episodes for pharmaceutical drugs with the exception of benzodiazepines, ranging from 26.0% for methadone to 49.3% for buprenorphine. Counselling was the most common main treatment type in episodes where benzodiazepines (28.9% of episodes) was the principal drug of concern. A filter allows the user to view data for main treatment type, reason for cessation or treatment delivery setting.
ABS 2011. Australian Standard Classification of Drugs of Concern, 2011. ABS cat. no. 1248.0. Canberra: ABS.
Department of Health 2017. National Drug Strategy 2017–2026. Canberra: Commonwealth of Australia.


