Health across socioeconomic groups
Citation
AIHW
Australian Institute of Health and Welfare (2022) Health across socioeconomic groups, AIHW, Australian Government, accessed 26 April 2024.
APA
Australian Institute of Health and Welfare. (2022). Health across socioeconomic groups. Retrieved from https://pp.aihw.gov.au/reports/australias-health/health-across-socioeconomic-groups
MLA
Health across socioeconomic groups. Australian Institute of Health and Welfare, 07 July 2022, https://pp.aihw.gov.au/reports/australias-health/health-across-socioeconomic-groups
Vancouver
Australian Institute of Health and Welfare. Health across socioeconomic groups [Internet]. Canberra: Australian Institute of Health and Welfare, 2022 [cited 2024 Apr. 26]. Available from: https://pp.aihw.gov.au/reports/australias-health/health-across-socioeconomic-groups
Harvard
Australian Institute of Health and Welfare (AIHW) 2022, Health across socioeconomic groups, viewed 26 April 2024, https://pp.aihw.gov.au/reports/australias-health/health-across-socioeconomic-groups
Get citations as an Endnote file: Endnote

On this page
Socioeconomic factors are key determinants of health. Having access to material and social resources and being able to participate in society are important for maintaining good health.
Generally, people in lower socioeconomic groups are at greater risk of poor health, have higher rates of illness, disability and death, and live shorter lives than people from higher socioeconomic groups (van Lenthe and Mackenbach 2021). The higher a person’s socioeconomic position, the healthier they tend to be – a phenomenon often termed the ‘social gradient of health’. In countries at all levels of income, health and illness follow a social gradient: the lower the socioeconomic position, the worse the health (WHO 2022). See Social determinants of health and Determinants of health for Indigenous Australians.
This page compares socioeconomic groups on health measures across 4 key health areas, focusing on people in the lowest and highest socioeconomic groups, where differences are usually large. It highlights that for almost all health measures, people from lower socioeconomic groups fare worse.
Measuring socioeconomic position – the Index of Relative Socio-economic Disadvantage
Socioeconomic position can be measured using an individual characteristic, such as a person’s level of income, education or occupation, or it may be constructed as a composite measure using a range of socioeconomic information.
In the AIHW’s reporting on health across socioeconomic groups, a composite measure of socioeconomic position known as the Index of Relative Socio-economic Disadvantage (IRSD) is frequently used (ABS 2018).
The IRSD classifies individuals according to the socioeconomic characteristics of the area in which they live. It scores each area by summarising attributes of the population, such as low income, low educational attainment, high unemployment and jobs in relatively unskilled occupations. Areas can then be ranked according to their score. The population living in the 20% of areas with the greatest overall level of disadvantage is described as the ‘lowest socioeconomic group’. The 20% at the other end of the scale – the top fifth – is described as the ‘highest socioeconomic group’.
Note that the IRSD reflects the overall or average level of disadvantage of the population of an area; it does not show how individuals living in the same area differ from each other in their socioeconomic position. Inequality estimates based on area-level measures of socioeconomic position will underestimate inequalities because of the substantial variation in socioeconomic position within areas (Mather et al. 2014).
Health risk factors
On most health risk factors, adults living in the areas with the greatest overall level of disadvantage (the lowest socioeconomic group) fared worse than adults living in areas with the least overall level of disadvantage (the highest socioeconomic group).
Based on the Australian Bureau of Statistics 2017–18 National Health Survey, after adjusting for age differences, it is estimated that, when compared with adults living in the highest socioeconomic areas, adults living in the lowest socioeconomic areas were:
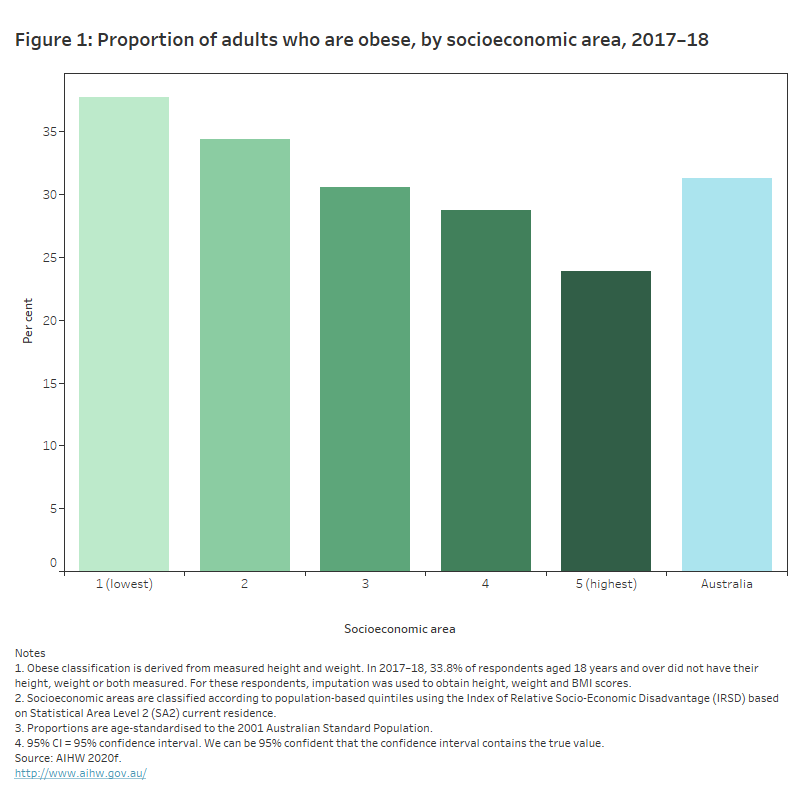
- 1.6 times as likely to be obese (38% and 24%) (AIHW 2020f) (Figure 1)
- 1.3 times as likely to be insufficiently active (63% and 48%) (AIHW 2020d)
- 1.2 times as likely to have uncontrolled high blood pressure (24% and 19%) (AIHW 2019).
The National Drug Strategy Household Survey 2019 used a similar composite measure of socioeconomic position, the Index of Relative Socioeconomic Advantage and Disadvantage (IRSAD). Based on the survey, it is estimated that, when compared with people aged 14 and over living in the highest socioeconomic areas, people aged 14 and over living in the lowest socioeconomic areas were:
- 3.6 times as likely to smoke daily (18% and 5.0%) (AIHW 2020e)
- at similar lifetime risk of harm from drinking alcohol (15% and 17%, with no difference between socioeconomic groups) (AIHW 2020e).
This chart shows that the proportion of adults who were obese in 2017–18 decreased across 5 socioeconomic groups – 38% of people living in the lowest socioeconomic areas were obese, compared with 24% of people living in the highest socioeconomic areas.
Chronic conditions
Rates of chronic conditions were also higher for people living in the lowest socioeconomic areas, compared with people living in the highest socioeconomic areas (ABS 2022b). In particular, it is estimated that, when compared with people living in the highest socioeconomic areas, people living in the lowest socioeconomic areas were:
- 2.0 times as likely to self-report having chronic obstructive pulmonary disease in 2017–18, among people aged 45 and over (7.1% and 3.6%) (AIHW 2020b)
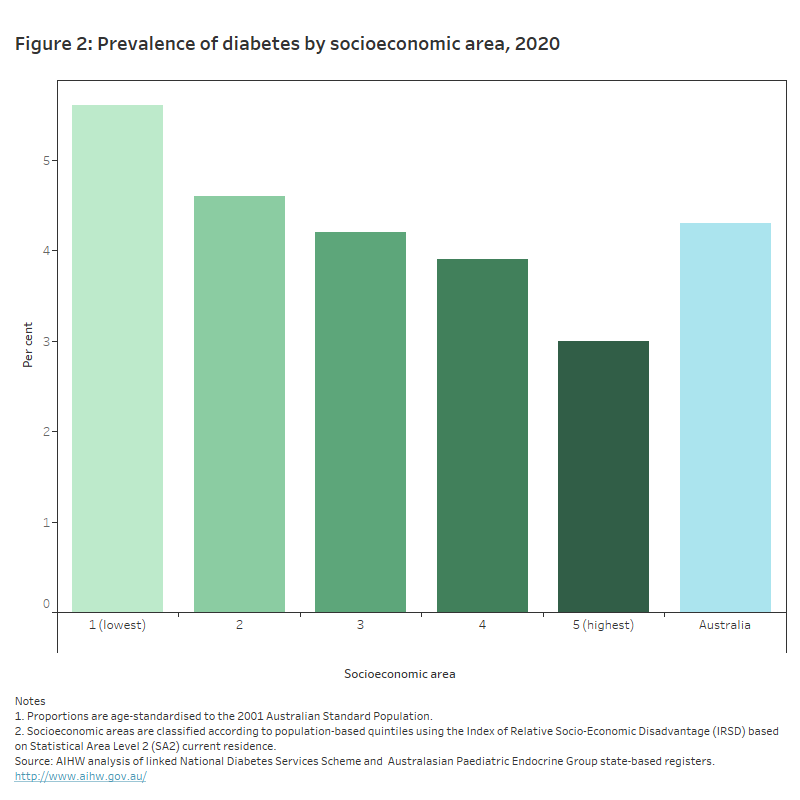
- 1.9 times as likely to have diabetes in 2020 (5.6% and 3.0%) (AIHW 2022a, 2020c) (Figure 2)
- 1.6 times as likely to have biomedical signs of chronic kidney disease in 2011–12, among adults (14% and 8.3%) (AIHW 2020a)
- 1.6 times as likely to self-report having coronary heart disease in 2017–18, among adults (3.2% and 2.0%) (AIHW 2021c)
- 1.1 times as likely to be newly diagnosed with cancer in 2012–2016 (509 and 484 cases per 100,000 population) (AIHW 2021b).
This chart shows that the prevalence of diabetes in 2020 decreased across 5 socioeconomic groups, from 5.6% of people living in the lowest socioeconomic areas to 3.0% of people living in the highest socioeconomic areas.
Deaths
For deaths occurring in 2020, people living in the lowest socioeconomic areas were 1.5 times as likely to die as people living in the highest socioeconomic areas (AIHW 2022).
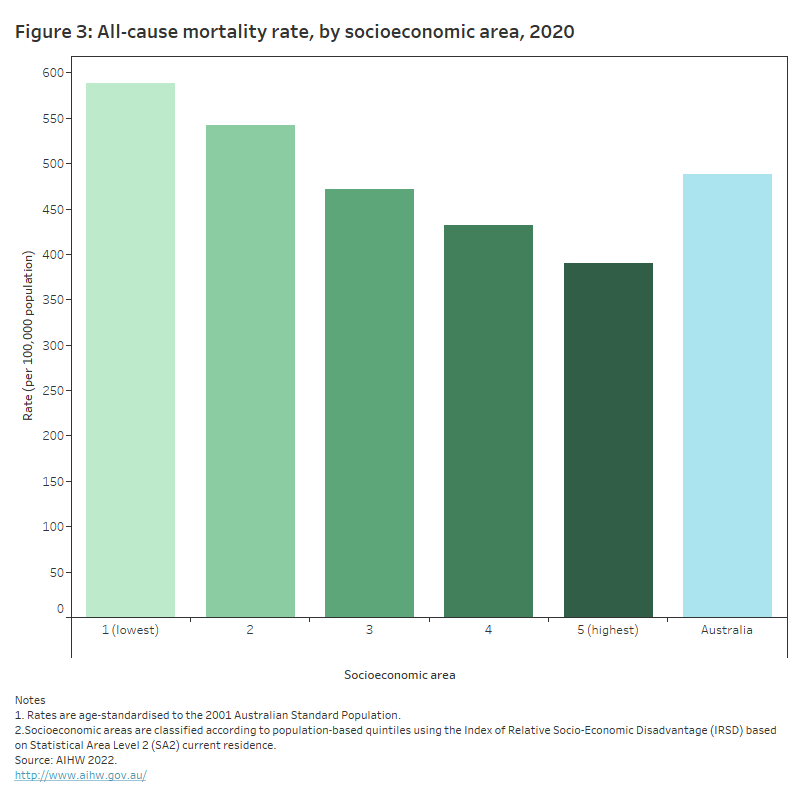
After adjusting for age differences in the population, the mortality rate from all causes of death for people living in the lowest socioeconomic areas was 589 deaths per 100,000 population, compared with 542 in the second group, 472 in the third, 432 in the fourth, and 390 for people living in the highest socioeconomic areas (Figure 3).
People living in the lowest socioeconomic areas were 2.2 times as likely to die from potentially avoidable causes in 2020 (140 and 65 deaths per 100,000 population) – a potentially avoidable death being a premature death that could have been avoided with timely and effective health care.
Disease-specific death rates were generally higher for people living in the lowest socioeconomic areas, compared with people living in the highest areas. In particular, when compared with people living in the highest socioeconomic areas, people in the lowest socioeconomic areas in 2016–2020 were:
- 2.6 times as likely to die from chronic obstructive pulmonary disease (33 and 13 deaths per 100,000 population)
- 2.0 times as likely to die from lung cancer (38 and 19 deaths per 100,000 population)
- 1.6 times as likely to die from coronary heart disease (70 and 43 deaths per 100,000 population)
- 1.3 times as likely to die from cerebrovascular disease (mostly stroke) (34 and 27 deaths per 100,000 population)
- 1.1 times as likely to die from dementia (including Alzheimer’s disease) (42 and 40 deaths per 100,000 population) (AIHW 2022).
This chart shows that the all-cause mortality rate in 2020 decreased across 5 socioeconomic groups, from 589 per 100,000 for people living in the lowest socioeconomic areas, to 390 per 100,000 for people living in the highest socioeconomic areas.
In 2018, males and females living in the lowest socioeconomic areas lived, on average, 5.9 and 3.9 years less than males and females living in the highest socioeconomic areas (AIHW 2021a).
See Life expectancy and causes of death and 'Chapter 2 Changes in the health of Australians during the COVID-19 period’ in Australia’s health 2022: data insights.
Burden of disease
Burden of disease analysis combines estimates of the fatal and non-fatal impact of disease. The ‘disability adjusted life year’ (DALY) measure combines health loss from living with illness and injury and dying prematurely to estimate the total burden of health loss (see Glossary and Burden of disease). One DALY is equivalent to one healthy year of life lost.
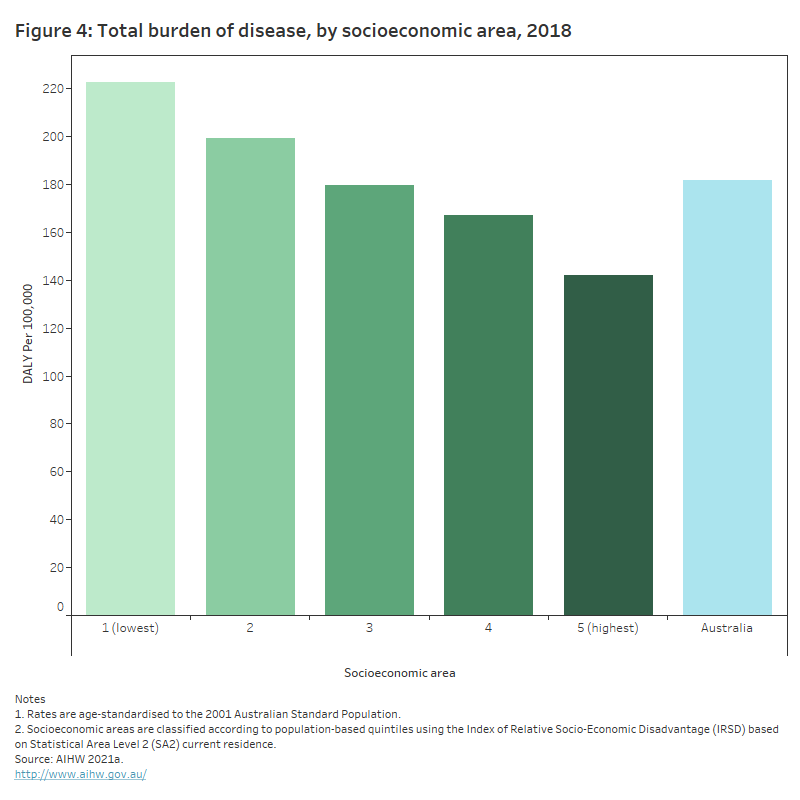
In 2018, total burden decreased with increasing socioeconomic group: total burden rates were 1.6 times as high for people living in the lowest socioeconomic areas (223 DALY per 1,000 population) as for people living in the highest socioeconomic areas (142 DALY per 1,000 population) (AIHW 2021a) (Figure 4).
Compared with people living in the highest socioeconomic areas, people living in the lowest socioeconomic areas experienced burden of disease that was estimated to be:
- 2.4 times as high for type 2 diabetes (5.8 and 2.4 DALY per 1,000 population)
- 2.2 times as high for lung cancer (7.4 and 3.3 DALY per 1,000 population)
- 2.0 times as high for coronary heart disease (15 and 7.2 DALY per 1,000 population)
- 1.6 times as high for stroke (5.2 and 3.3 DALY per 1,000 population)
- 1.2 times as high for dementia (6.6 and 5.7 DALY per 1,000 population).
In terms of population impact, if all Australians had experienced the same burden as people living in the highest socioeconomic areas in 2018, the total disease burden could have been reduced by one-fifth (21%) (AIHW 2021a).
This chart shows that the total burden of disease in 2018 decreased across 5 socioeconomic groups, from 223 DALY per 1,000 for people living in the lowest socioeconomic areas to 142 DALY per 1,000 for people living in the highest socioeconomic areas.
Impact of COVID-19 across socioeconomic groups
As with most other diseases, COVID-19 disproportionately affects lower socioeconomic groups. Of the 2,639 COVID-19 deaths that occurred by 30 April 2022, there were more than 3 times as many among people living in the lowest socioeconomic areas compared with people living in the highest socioeconomic areas (1,870 and 527 deaths) (ABS 2022a). Age-standardised mortality rates were 2.8 times as high (105 and 38 per million) (AIHW 2021d).
For more information on the health impact of the pandemic, see ‘Chapter 1 The impact of a new disease: COVID-19 from 2020, 2021 and into 2022’ and ‘Chapter 2 Changes in the health of Australians during the COVID-19 period’ in Australia’s health 2022: data insights.
Where do I go for more information?
For more information on health across socioeconomic groups, see:
- Mortality Over Regions and Time (MORT) books
- Australian Burden of Disease Study: impact and causes of illness and death in Australia 2018
References
ABS (Australian Bureau of Statistics) (2018) Census of population and housing: Socio-Economic Indexes for Areas (SEIFA), Australia, 2016, ABS, Australian Government, accessed 9 February 2022.
ABS (2022a) COVID-19 mortality in Australia: Deaths registered until 30 April 2022, ABS, Australian Government, accessed 27 May 2022.
ABS (2022b) Health conditions prevalence, ABS, Australian Government, accessed 21 March 2022.
AIHW (Australian Institute of Health and Welfare) (2019) High blood pressure, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2020a) Chronic kidney disease, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2020b) Chronic obstructive pulmonary disease, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2020c) Diabetes, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2020d) Insufficient physical activity, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2020e) National Drug Strategy Household Survey 2019, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2020f) Overweight and obesity: an interactive insight, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2021a) Australian Burden of Disease Study: impact and causes of illness and death in Australia 2018, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2021b) Cancer in Australia 2021, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2021c) Heart, stroke and vascular disease - Australian facts, AIHW, Australian Government, accessed 9 February 2022.
AIHW (2021d) 'The impact of a new disease: COVID-19 from 2020, 2021 and into 2022', in Australia’s health 2022: data insights, AIHW, Australian Government, accessed 27 May 2022.
AIHW (2022a) AIHW analysis of linked National Diabetes Services Scheme and Australian Paediatric Endocrine Group state-based registries, AIHW, Australian Government.
AIHW (2022b) MORT (Mortality Over Regions and Time) books: Socioeconomic group, 2016–2020, AIHW, Australian Government, accessed 27 May 2022.
Mather T, Banks E, Joshy G, Bauman A, Phongsavan P and Korda RJ (2014) Variation in health inequalities according to measures of socioeconomic status and age, Australian and New Zealand Journal of Public Health, 38(5):436–440, doi:10.1111/1753-6405.12239.
van Lenthe F and Mackenbach JP (2021) ‘Socioeconomic inequalities in health in high-income countries: the facts and the options’, in Detels R, Karim QA, Baum F, Li L and Leyland AH (eds) Oxford textbook of global public health, 7th edn, Oxford University Press, Oxford.
WHO (World Health Organization) (2022) Social determinants of health, WHO, accessed 17 January 2022.


