Health workforce
Citation
AIHW
Australian Institute of Health and Welfare (2022) Health workforce, AIHW, Australian Government, accessed 27 April 2024.
APA
Australian Institute of Health and Welfare. (2022). Health workforce. Retrieved from https://pp.aihw.gov.au/reports/workforce/health-workforce
MLA
Health workforce. Australian Institute of Health and Welfare, 07 July 2022, https://pp.aihw.gov.au/reports/workforce/health-workforce
Vancouver
Australian Institute of Health and Welfare. Health workforce [Internet]. Canberra: Australian Institute of Health and Welfare, 2022 [cited 2024 Apr. 27]. Available from: https://pp.aihw.gov.au/reports/workforce/health-workforce
Harvard
Australian Institute of Health and Welfare (AIHW) 2022, Health workforce, viewed 27 April 2024, https://pp.aihw.gov.au/reports/workforce/health-workforce
Get citations as an Endnote file: Endnote
On this page:
The health workforce in Australia is large and diverse, covering many occupations. These include health practitioners registered with the Australian Health Practitioner Regulation Agency (Ahpra) as well as other health professionals and health support workers. Due to data limitations regarding the other professional groups, this page presents information on the health practitioners who were registered with Ahpra.
The Australian Health Practitioner Regulation Agency
Ahpra is the statutory authority responsible for administering the National Registration and Accreditation Scheme (Ahpra 2021c).
The current list of registered health professions includes Aboriginal and Torres Strait Islander health practitioners, chiropractors, Chinese medicine practitioners, medical radiation practitioners, occupational therapists, optometrists, osteopaths, paramedicine practitioners, pharmacists, physiotherapists, podiatrists, psychologists, oral health therapists, dental hygienists, dental therapists, dental prosthetists, dentists, nurses, midwives, and medical practitioners.
The AIHW derives estimates of the Australian health workforce using the categories of 15 health professions from the Health Workforce Data Tool of the Australian Department of Health (Department of Health 2021b). Health professionals may be registered in more than one profession with Ahpra. All Ahpra numbers reported refer to registered health professionals who are employed in Australia and working in their registered profession, Ahpra-registered professionals who are not in the labour force are excluded.
Overview of registered health professionals
There were more than 642,000 health practitioners working in their registered professions in Australia in 2020, which includes 105,300 medical practitioners, 350,000 nurses and midwives, 21,500 dental practitioners, and 166,000 allied health professionals (Table 1).
Trends
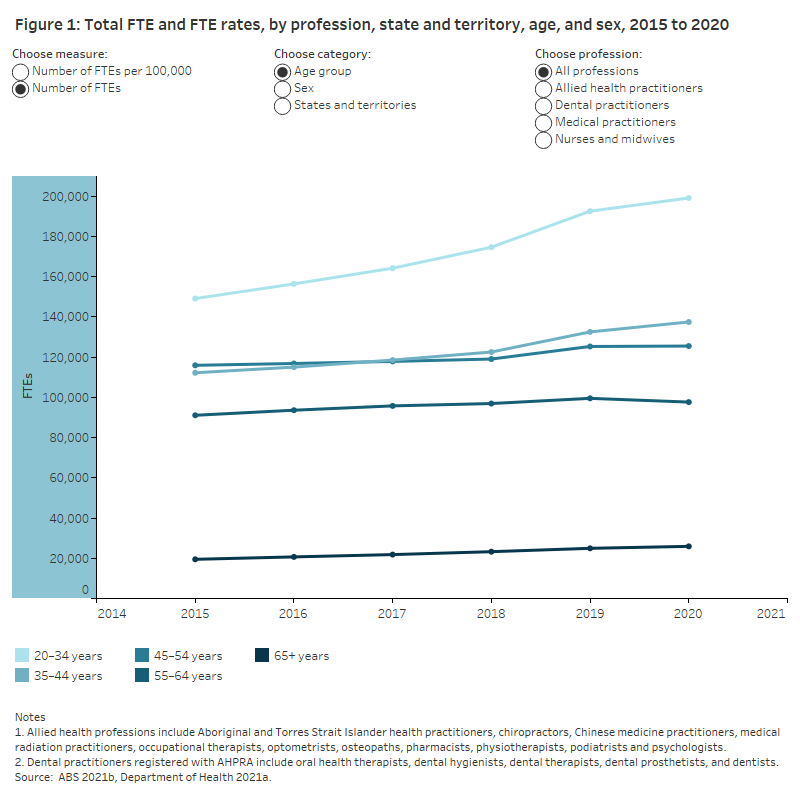
On this page, health professions are categorised into 4 profession groups: allied health, dental practitioners, medical practitioners, and nurses and midwives. Between 2015 and 2020 the Australian registered health workforce increased by more than 110,500 professionals. The number of full-time equivalent (FTE) health professionals per 100,000 population (FTE rate) rose steadily for each profession group between 2015 and 2020 (Figure 1).
Nurses and midwives continued to be the largest group of registered health professionals in Australia, at about 350,000 registered in 2020 (54% of all registered health professionals).
Relative to the Australian population, allied health workers showed the greatest growth in FTE rate from 2015 to 2020 (an increase of 147 FTE per 100,000 people). Note that the inclusion of paramedicine practitioners as a new registered health profession (since 2019) has contributed to this increase, accounting for 78 FTE per 100,000 people in 2020.
| Profession | Measure | 2015 | 2020 | % change |
|---|---|---|---|---|
|
Allied health (a) |
Number of practitioners |
118,418 |
166,048 |
40.2 |
|
FTE total |
106,500 |
152,559 |
43.2 |
|
|
FTE per 100,000 population |
447 |
594 |
32.9 |
|
|
Dental practitioners (b) |
Number of practitioners |
19,051 |
21,549 |
13.1 |
|
FTE total |
17,613 |
19,450 |
10.4 |
|
|
FTE per 100,000 population |
74 |
76 |
2.7 |
|
|
Medical practitioners |
Number of practitioners |
87,999 |
105,293 |
19.7 |
|
FTE total |
93,356 |
107,777 |
15.4 |
|
|
FTE per 100,000 population |
392 |
420 |
7.0 |
|
|
Nurses and midwives |
Number of practitioners |
306,487 |
349,589 |
14.1 |
|
FTE total |
270,368 |
305,855 |
13.1 |
|
|
FTE per 100,000 population |
1,135 |
1,191 |
4.9 |
|
|
All professions |
Number of practitioners |
531,955 |
642,479 |
20.8 |
|
FTE total |
487,837 |
585,642 |
20.0 |
|
|
FTE per 100,000 population |
2,048 |
2,280 |
11.3 |
Notes
(a) For the purpose of this page, allied health professions include Aboriginal and Torres Strait Islander health practitioners, chiropractors, Chinese medicine practitioners, medical radiation practitioners, occupational therapists, optometrists, osteopaths, pharmacists, physiotherapists, podiatrists, psychologists, and paramedicine practitioners. In 2019, paramedicine practitioners emerged as a new career path of registered health professionals in Australia.
(b) Dental practitioners registered with Ahpra include oral health therapists, dental hygienists, dental therapists, dental prosthetists, and dentists.
(c) Under the Health Practitioner Regulation National Law 2009, a medical practitioner is a person who holds registration with the Medical Board of Australia.
Source: ABS 2021a; APHRA 2021; Department of Health 2021b.
Demographics
On average, Australia’s health workforce is predominantly female (except for medical and dental practitioners), and aged 20–34. However, there have been some notable changes between 2015 and 2020. There are more young health professionals in the health workforce, and the proportion of female medical and dental practitioners has risen (Figure 1).
Age
Between 2015 and 2020:
- The FTE rate of all health professionals aged 20–34 and 35–44 increased by 24% (from 626 to 775 FTE per 100,000 people) and 14% (from 471 to 535 FTE per 100,000 people), respectively, compared to the FTE rates of health professionals aged 45–54 and 55–64 which were almost unchanged over the same period.
- The FTE rate of nurses and midwives and allied health practitioners aged 20–34 increased by 24% (from 310 to 383 FTE per 100,000 people) and 31% (from 192 to 252 FTE per 100,000 people), respectively.
Sex
Between 2015 and 2020:
- The FTE rate of health professionals that are women remains at around 2.4 times that of men in 2020.
- While there are more men than women among medical and dental practitioners, the FTE rate of female medical and dental practitioners increased by 18% (from 143 to 169 FTE per 100,000 people) and 12% (from 32 to 36 FTE per 100,000 people) respectively, compared to the FTE rate for male medical practitioners which increased slightly by 1% (from 249 to 251 FTE per 100,000 people) and the FTE rate for dental practitioners which decreased by 5% (from 41 to 39 FTE per 100,000 people).
In 2020:
- The female/male ratio of the overall number of health professionals was 2.9, with a total of 476,500 women and 166,000 men registered and employed in Australia’s health workforce.
- The FTE rate of females was 6.8 times that of males for nurses and midwives, and 1.7 times for allied health practitioners.
Jurisdiction
Between 2015 and 2020:
- Northern Territory had the highest number of registered health professionals relative to its population (2,898 FTE per 100,000 people in 2020) thanks to its high rate of nurses and midwives, and medical practitioners.
- Northern Territory also had the lowest dental practitioner FTE rate over this period (48 FTE per 100,000 people compared with 76 per 100,000 in South Australia).
- New South Wales had the lowest FTE rate for all professions (2,132 FTE per 100,000 people in 2020).
The graphs show that the health workforce is getting younger (24% increase in FTE rate of 20- to 34-year-old health professionals); that there is increasing numbers of female medical and dental practitioners in the 2015-2020 period; and that the Northern Territory had the highest number of health professionals relative to its population in 2020 (2,898 FTEs per 100,000 people).
Rural and remote areas
The accessibility of Australia’s health workforce is highly dependent on the distribution of its members in areas where they are most needed. In this section, the clinical FTE rate is used, in contrast with the FTE rates discussed above. The clinical FTE rate indicates the full-time equivalent number of health professionals working clinical hours relative to the population.
For all registered professions, the number of employed FTE clinicians working in their registered professions decreased with increasing remoteness, a trend seen each year since 2015 (Figure 2). There were also more registered clinical FTE health professionals in Major cities than in all regional and remote areas of Australia combined. In 2020, there were more than 386,000 FTE clinicians working in Major cities compared with 132,000 in all other remoteness areas.
Relative to the populations in these areas, Major cities had a greater number of working FTE clinicians (2,077 clinical FTE per 100,000 people in 2020) than each of the other remoteness areas. For the other remoteness areas:
- Inner regional areas had 1,890 FTE per 100,000 people.
- Outer regional areas had 1,761 FTE per 100,000 people.
- Remote areas had 1,959 FTE per 100,000 people.
- Very remote areas had 1,833 FTE per 100,000 people.
The number of FTEs and FTE rate of all health professionals decreased with remoteness, a pattern consistently seen from 2015 to 2020. For nurses and midwives, however, remote and very remote areas (1,187 and 1,202 FTEs per 100,000 people, respectively, in 2020) had a greater FTE rate compared with major cities (1,069 FTEs per 100,000 people in 2020).
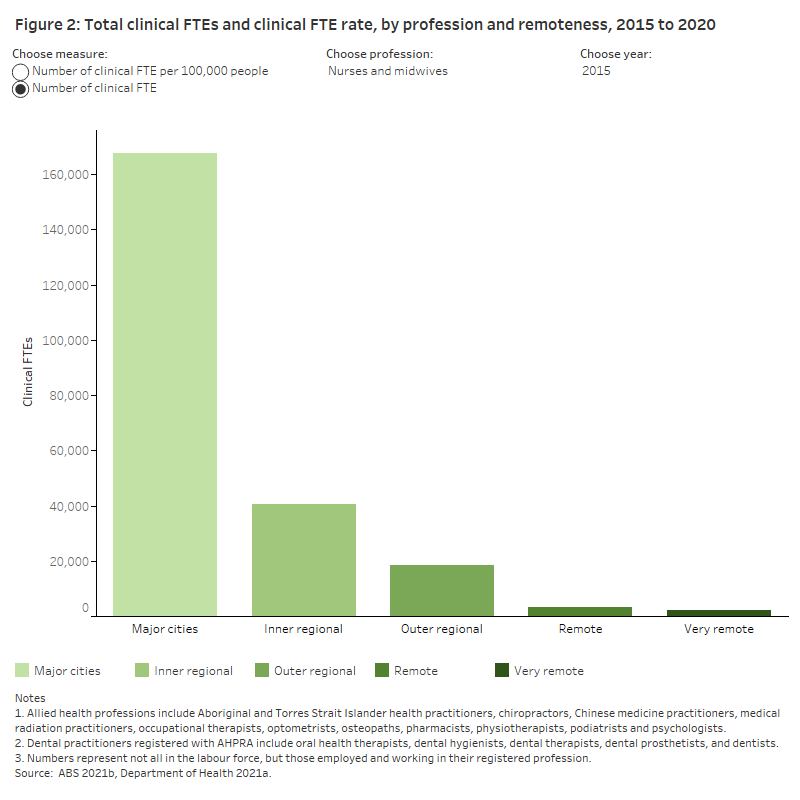
This trend is also seen when looking at each of the health profession groups, except for nurses and midwives. Both Remote and Very remote areas have a greater number of registered and working clinical FTE nurses and midwives relative to the population in these areas. In 2020, there were 1,202 FTE clinical nurses and midwives per 100,000 people in Very remote areas compared with 1,069 in Major cities.
Despite having relatively high clinical FTE rate, people living in remote areas and very remote areas generally have poorer access to health service than people in regional areas and Major cities (AIHW 2018). Australian people living in remote areas may need to travel long distances or relocate to attend health services or receive specialised treatment. Medicare claims data from 2017–18 also indicated that rural and remote populations rely more on general practitioners to provide health care services, due to less availability of local specialist services (AIHW 2019). Also, in the early stages of COVID‐19 pandemic, the capacity of remote health services to maintain workforce was curtailed due to border restrictions imposed by state/territory, and Australian government in order to reduce domestic and international travel. Many remote health services were unable to source previously used interstate and international trained nurses and doctors who possess remote health service knowledge and experience and have established relationships with remote communities (Fitts et al. 2020).
According to reports published by Medical Deans Australia and New Zealand (MDANZ), using the Medical Schools Outcomes Database, graduating medical students have shown consistent preference for practising in capital cities. In 2020, 65% of surveyed medical students indicated a preference to work in capital cities (Table 2). In contrast, only 17% of students indicated a preference to work in regional cities, small towns, or small communities (MDANZ 2021).
| Year | First preference region of future practice | Capital city | Major urban centre | Regional city or large town | Smaller town | Small community | Total |
|---|---|---|---|---|---|---|---|
|
2015 |
Number |
1,240 |
367 |
231 |
84 |
36 |
1,958 |
|
2015 |
Per cent |
63.3 |
18.7 |
11.8 |
4.3 |
1.8 |
100 |
|
2016 |
Number |
1,330 |
352 |
260 |
94 |
32 |
2,068 |
|
2016 |
Per cent |
64.3 |
17.0 |
12.6 |
4.5 |
1.5 |
100 |
|
2017 |
Number |
1,271 |
347 |
252 |
83 |
34 |
1,987 |
|
2017 |
Per cent |
64.0 |
17.5 |
12.7 |
4.2 |
1.7 |
100 |
|
2018 |
Number |
1,328 |
374 |
271 |
85 |
27 |
2,085 |
|
2018 |
Per cent |
64.2 |
17.5 |
12.9 |
4.1 |
1.3 |
100 |
|
2019 |
Number |
1,286 |
364 |
226 |
65 |
26 |
1,967 |
|
2019 |
Per cent |
65.4 |
18.5 |
11.5 |
3.3 |
1.3 |
100 |
|
2020 |
Number |
1,084 |
288 |
197 |
68 |
23 |
1,660 |
|
2020 |
Per cent |
65.3 |
17.3 |
11.9 |
4.1 |
1.4 |
100 |
Source: MDANZ 2021.
Occupations working the most hours
The FTE number is calculated based on the total hours worked in a ‘standard working week’, which may change depending on occupation. For example, a standard working week for medical practitioners is considered to be 40 hours, and 38 hours for nurses and midwives, dental practitioners and allied health professionals. The ratio of FTEs relative to the number of health professionals therefore provides an overall indication of whether occupational groups worked longer or less than their standard hours.
Between 2015 and 2020, medical practitioners were the only occupational group whose total FTE was greater than the number of practitioners, indicating that medical practitioners overall worked more than their FTE of 40 hours a week (Table 1). This contrasts with allied health practitioners, nurses and midwives, and dental practitioners, where the total number of practitioners exceeded total FTEs over the same period. This may indicate increasingly part-time arrangements for these practitioners.
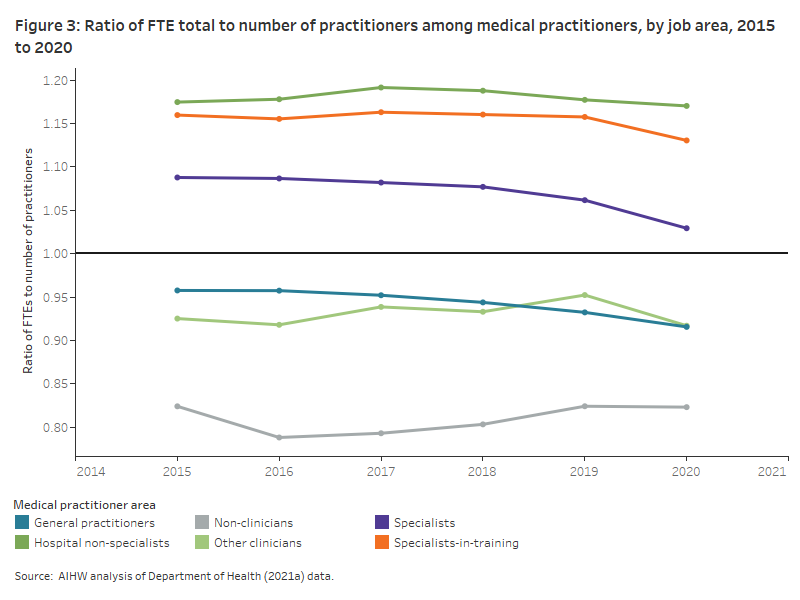
Overall, medical practitioners, specialists, specialists-in-training, and hospital non-specialists worked longer hours (ratio was greater than 1) than their full-time equivalent (Figure 3).
Among specialists, specialists-in-training and hospital non-specialists, the ratio of total FTEs to number of practitioners was greater than 1 from 2015 to 2020 indicating that these medical practitioners overall are working longer than their full-time obligation. Over the same period, general practitioners, other clinicians and non-clinicians had an FTE to number of practitioners ratio less than 1, indicating these health professionals worked less hours than their full-time obligation with non-clinicians working the shortest hours.
Non-registered health professions
Many people employed in the health sector work in occupations that are not registered by Ahpra and there are fewer available data for these groups. These members of the health workforce still play an important role in delivering health services to Australians and include, for example, dieticians, clerical workers, health information managers, welfare professionals, service workers, cleaners, and gardeners. Also, some health professionals (such as dietician, audiologist, speech pathologist, etc.) are self-regulated by their professional association to ensure that high safety and quality standards are maintained.
According to the Australian Bureau of Statistics (ABS) 2016 Census of Population and Housing – more than 820,000 people reported working in the health services industry (ABS 2021a). Outside of the Ahpra-registered professions, this included around 13,200 ambulance officers and paramedics (note that paramedicine practitioners were then listed as a new registered health profession in 2019 data); 21,000 medical technicians; 21,000 dental assistants; and 26,100 nursing support and personal care workers. The ABS will complete the 2021 Census of Population and Housing in June 2022 (ABS 2021b).
Impact of the COVID-19 pandemic on the health workforce
At the time of writing, the COVID-19 pandemic continues. Many of Australia’s healthcare workforce are on the frontline and continue to be impacted by the pandemic in different ways. However, as data related to COVID-19 impacts are limited and obtained from small-sized surveys, the following results should be interpreted with caution.
The pandemic has affected the physical health of workers. A report of 2,163 healthcare workers during January and September 2020 indicated that in the second wave of the pandemic, when there was heightened community transmission, health care workers were more likely to be infected in the workplace and nurses were more likely to be infected than staff in other roles (Rafferty et al. 2021). Quigley et al. (2021) using data from January to July 2020 of 36 hospital outbreaks concluded that the infection rate of health workers was 2.7 times higher than community infection.
In terms of mental health, healthcare workers exhibit higher rates of anxiety, depression and suicidal ideation when compared to the general population (Beyondblue 2019). During emergencies like we have experienced during COVID-19, increased posttraumatic stress disorder (PTSD), anxiety and depression could be observed in healthcare workers (Shah et al. 2020). Some pandemic-related stress on healthcare workers is also evident (Aggar et al. 2021; Dobson et al. 2020; Holton et al. 2021; Pascoe et al. 2021; Smallwood et al. 2021a).
Some evidence suggested that the pandemic had increased the workload of health workers. An online survey of 7,846 frontline health workers conducted by Smallwood et al. (2021b) between August and October 2020 indicated that 21.5% increased their unpaid work hours, 20.8% of respondents increased their paid work hours, 16.8% were redeployed to a new work area, and 27.3% changed their work role.
Between 2015 and 2019, the share of foreign-trained doctors and nurses were almost unchanged (32% and 18% respectively, see OECD 2022). However, the international travel restrictions due to the pandemic might affect these shares. This is to be confirmed when updated data become available.
Some of the measures used to cope with COVID-19 in the healthcare sector
Pandemic response sub-register
At the onset of COVID-19, the Ahpra and the relevant National Boards established a temporary pandemic response sub-register up to 12 months in April 2020 (the 2020 sub-register) to help fast track the return to the workforce of experienced and qualified health practitioners. In early April 2021, the Commonwealth Health Minister requested that medical practitioners, nurses, midwives, and pharmacists be extended to stay on the sub-register for up to 12 months (to 5 April 2022) to help with the COVID-19 vaccination program only. This was also the case for Aboriginal and Torres Strait Islander Health Practitioners. On 8 September 2021, the registration of practitioners on the 2020 sub-register was changed so they could work in any area supporting the COVID-19 response. On 22 September 2021, Ahpra and the relevant National Boards established a new sub-register (the 2021 sub-register), for practitioners in 12 regulated health professions to return to practice for up to 12 months, working to the full scope of their registration. As of 22 December 2021, there were 23,307 health professionals on the 2020 pandemic response sub-register and 20,860 health professionals on the 2021 pandemic response sub-register (Ahpra 2021b).
Inclusion of Telehealth in Medicare Benefits Schedule
In March 2020, the Australian Government introduced new Medicare Benefits Schedule (MBS) funding so that specialists (and other clinicians) could provide telehealth consultations. Compared to the pre-existing funding, access to COVID-19 MBS telehealth funding was not geographically restricted. MBS reimbursement of specialist telehealth consultations was further extended to include telephone consultations in addition to video consultations. The temporary MBS telehealth items are available to general practitioners, medical practitioners, specialists, consultant physicians, nurse practitioners, participating midwives, allied health providers and dental practitioners in the practice of oral and maxillofacial surgery (Department of Health 2021a). From 1 January 2022, patient access to telehealth services has been supported by ongoing MBS arrangements which enable all Medicare eligible Australians to access telehealth (video and phone) services for a range of (out of hospital) consultations that can also be provided in person (Department of Health 2021c). Between March 2020 and December 2021, 87 million telehealth services were delivered to 16.2 million patients, with more than $4.4 billion in benefits paid and 89,180 practitioners having now used telehealth services (Australian Digital Health Agency 2021).
Mental Health support for healthcare workers
The Australian Government also funds tailored mental health supports for the health workforce. This includes implementing Every Doctor, Every Setting, a national framework to deliver a coordinated approach to support the mental health of doctors and medical students; The Essential Network (TEN) project, a multifaceted e-health hub, delivered by the Black Dog Institute for healthcare professionals by healthcare professionals; and DRS4DRS service which provides mental health consultations for doctors and medical students.
Elective surgery restrictions
Following a decision by National Cabinet, in the context of ensuring the health system maintained adequate capacity to deal with the COVID-19 pandemic, restrictions were applied to selected elective surgeries from 26 March 2020.
Under these restrictions, only Category 1 and exceptional Category 2 procedures could be undertaken. These restrictions were eased (but not fully lifted) from 29 April 2020, allowing all Category 2 and some important Category 3 procedures to be performed. In early January 2022, to help hospitals respond to the increasing number of patients with Omicron strain COVID-19, some states and territories such as New South Wales, Victoria, Queensland, South Australia reapplied temporary elective surgery suspensions (New South Wales Government 2022; Victoria Department of Health 2022; Queensland Government 2022; South Australia 2022). These restrictions resulted in delays to many types of elective surgery, waiting times for most intended procedures increased. The proportion of patients waiting more than 365 days for their elective surgery rose between 2019–20 and 2020–21 overall from 2.8% to 7.6% (AIHW 2021).
Where do I go for more information?
For more information on the health workforce, see:
- Department of Health’s Health workforce data tool
- MDANZ’s Medical schools outcomes database reports
- Australian Bureau of Statistics (ABS) 2016 Census of Population and Housing (need to register, “Employment, Income and Education/Health Care and Social Assistance” section)
Visit Workforce for more on this topic.
ABS (Australian Bureau of Statistics) (2021a) ABS Census TableBuilder, ABS, Australian Government, accessed 10 January 2022 (need to register).
ABS (2021b) 2021 Census topics and data release plan, ABS, Australian Government, accessed 10 January 2022.
ABS (2021c) Regional population growth, Australia, 2019–20 financial year, ABS, Australian Government, accessed 10 January 2022.
ADHA (Australian Digital Health Agency) (2021) Telehealth, ADHA, Australian Government, accessed 8 January 2022.
Aggar C, Samios C, Penman O, Whiteing N, Massey D, Rafferty R, Bowen K and Stephens A (2022) ‘The impact of COVID‐19 pandemic‐related stress experienced by Australian nurses’, International Journal of Mental Health Nursing, 31(1):91–103, doi:10.1111/inm.12938.
Ahpra (Australian Health Practitioner Regulation Agency) (2021a) Legislation, Ahpra, accessed 20 January 2022.
Ahpra (2021b) Pandemic response sub-registers, Ahpra, accessed 8 January 2022.
Ahpra (2021c) Who we are, Ahpra, accessed 23 December 2021.
AIHW (Australian Institute of Health and Welfare) (2018) Survey of health care: selected findings for rural and remote Australians, AIHW, Australian Government, accessed 15 February 2022.
AIHW (2019) Rural & remote health, AIHW, Australian Government, accessed 15 February 2022.
AIHW (2021) Elective surgery, AIHW, Australian Government, accessed 1 February 2022.
Beyondblue (2019) National mental health survey of doctors and medical students, Beyondblue, accessed 27 April 2022.
Department of Health (2021a) COVID-19 temporary MBS Telehealth services, Department of Health, Australian Government, accessed 8 January 2021.
Department of Health (2021b) Health workforce data tool, Department of Health, Australian Government, accessed 8 January 2021.
Department of Health (2021c) MBS Telehealth services from 1 January 2022, Department of Health, Australian Government, accessed 8 January 2021.
Dobson H, Malpas CB, Burrell AJ, Gurvich C, Chen L, Kulkarni J and Winton-Brown T (2021) ‘Burnout and psychological distress amongst Australian healthcare workers during the COVID-19 pandemic’, Australasian Psychiatry, 29(1):26–30, doi:10.1177/1039856220965045.
Fitts MS, Russell D, Mathew S, Liddle Z, Mulholland E, Comerford C and Wakerman J (2020) ‘Remote health service vulnerabilities and responses to the COVID‐19 pandemic’, Australian Journal of Rural Health, 28(6), 613–617, doi:10.1111/ajr.12672.
Government of South Australia (2022) Limitations to surgical treatment (elective surgery), Government of South Australia, accessed 1 February 2022.
Holton S, Wynter K, Trueman M, Bruce S, Sweeney S, Crowe S, Dabscheck A, Eleftheriou P, Booth S, Hitch D and Said CM (2021) ‘Immediate impact of the COVID-19 pandemic on the work and personal lives of Australian hospital clinical staff’, Australian Health Review, 45(6), 656–666, doi:10.1071/AH21014.
MDANZ (Medical Deans Australia and New Zealand) (2021) National data report 2021, MDANZ, accessed 15 December 2021.
NSW Government (2022) Staged return of non-urgent elective surgery, NSW Government, accessed 1 February 2022.
OECD (Organisation for Economic Co-operation and Development) (2022) Health Workforce Migration, Health statistics, OECD, accessed 27 April 2022.
Pascoe A, Paul E, Johnson D, Putland M, Willis K and Smallwood N (2021) ‘Differences in coping strategies and help-seeking behaviours among Australian junior and senior doctors during the COVID-19 pandemic’, International Journal of Environmental Research and Public Health, 18(24):13275, doi:10.3390/ijerph182413275.
Queensland Government (2022) Non-urgent elective surgeries postponed, Queensland Government, accessed 1 February 2022.
Quigley AL, Stone H, Nguyen PY, Chughtai AA and MacIntyre CR (2021) ‘Estimating the burden of COVID-19 on the Australian healthcare workers and health system during the first six months of the pandemic’, International Journal of Nursing Studies, 114:1–11, doi:10.1016/j.ijnurstu.2020.103811.
Rafferty AC, Hewitt MC, Wright R, Hogarth F, Coatsworth N, Ampt F, Dougall S, Alpren C, Causer L, Coffey C, Wakefield A, Campbell S, Pingault N, Harlock M, Smith KJ and Kirk MD (2021) ‘COVID-19 in health care workers, Australia 2020’, Communication Disease Intelligence, 45:1–11, doi:10.33321//cdi.2021.45.57.
Shah K, Kamrai D, Mekala H, Mann B, Desai K and Patel RS (2020) ‘Focus on mental health during the Coronavirus (COVID-19) pandemic: Applying learnings from the past outbreaks’, Cureus 12(3): e7405, doi:10.7759/cureus.7405.
Smallwood N, Karimi L, Bismark M, Putland M, Johnson D, Dharmage SC, Barson E, Atkin N, Long C, Ng I and Holland A (2021a) ‘High levels of psychosocial distress among Australian frontline healthcare workers during the COVID-19 pandemic: a cross-sectional survey’, General Psychiatry, 34(5): e100577, doi:10.1136/gpsych-2021-100577.
Smallwood N, Pascoe A, Karimi L, Bismark M and Willis K (2021b) ‘Occupational disruptions during the COVID-19 pandemic and their association with healthcare workers’ mental health’, International Journal of Environmental Research and Public Health, 18(17):9263, doi:10.3390/ijerph18179263.
Victoria Department of Health (2022) Changes to non-urgent surgery settings helping hospitals respond to Omicron, Victoria Department of Health, accessed 1 February 2022.
Amendments
23 November 2022 – Under the ‘Non-registered health professions’ heading, the text has been changed from:
'According to the Australian Bureau of Statistics (ABS) 2016 Census of Population and Housing – more than 820,000 people reported working in the health services industry (ABS 2021a). Outside of the Ahpra-registered professions, this included around 13,200 ambulance officers and paramedics; 21,000 medical technicians; 21,000 dental assistants; and 26,100 nursing support and personal care workers. The ABS will complete the 2021 Census of Population and Housing in June 2022 (ABS 2021b).'
To:
'According to the Australian Bureau of Statistics (ABS) 2016 Census of Population and Housing – more than 820,000 people reported working in the health services industry (ABS 2021a). Outside of the Ahpra-registered professions, this included around 13,200 ambulance officers and paramedics (note that paramedicine practitioners were then listed as a new registered health profession in 2019 data); 21,000 medical technicians; 21,000 dental assistants; and 26,100 nursing support and personal care workers. The ABS will complete the 2021 Census of Population and Housing in June 2022 (ABS 2021b).'


