Alcohol and other drug treatment services
Citation
AIHW
Australian Institute of Health and Welfare (2023) Alcohol and other drug treatment services, AIHW, Australian Government, accessed 27 April 2024.
APA
Australian Institute of Health and Welfare. (2023). Alcohol and other drug treatment services. Retrieved from https://pp.aihw.gov.au/reports/alcohol-other-drug-treatment-services/alcohol-and-other-drug-treatment-services
MLA
Alcohol and other drug treatment services. Australian Institute of Health and Welfare, 20 April 2023, https://pp.aihw.gov.au/reports/alcohol-other-drug-treatment-services/alcohol-and-other-drug-treatment-services
Vancouver
Australian Institute of Health and Welfare. Alcohol and other drug treatment services [Internet]. Canberra: Australian Institute of Health and Welfare, 2023 [cited 2024 Apr. 27]. Available from: https://pp.aihw.gov.au/reports/alcohol-other-drug-treatment-services/alcohol-and-other-drug-treatment-services
Harvard
Australian Institute of Health and Welfare (AIHW) 2023, Alcohol and other drug treatment services, viewed 27 April 2024, https://pp.aihw.gov.au/reports/alcohol-other-drug-treatment-services/alcohol-and-other-drug-treatment-services
Get citations as an Endnote file: Endnote
On this page:
Alcohol and other drug (AOD) use is linked to increased risk of injury, mental illness, preventable disease, road trauma and death (AIHW 2021). AOD treatment agencies across Australia provide a range of services and support to people receiving treatment for their own drug use, as well as their families and friends.
Many types of treatment are available in Australia to assist people with drug and alcohol use. Most treatments aim to reduce harm, coordinate care, and provide intensive interventions (for example, withdrawal management (detoxification); psycho–social counselling; rehabilitation; and pharmacotherapy). Reducing harm from alcohol, tobacco and other drugs may include ceasing use, reducing use, or changing use patterns to be less harmful (including reducing the severity of dependence) (Department of Health and Aged Care 2019).
Opioid pharmacotherapy (see glossary) is a type of treatment that can reduce drug cravings and other withdrawal symptoms in people experiencing opioid drug dependence (such as codeine or heroin dependence).
See Alcohol and Illicit use of drugs for information on use of alcohol and other drugs.
Data sources
- Alcohol and Other Drug Treatment Services National Minimum Data Set (AODTS NMDS): provides information about publicly funded alcohol and other drug treatment services in Australia, the people they treat, and the treatment provided.
- National Opioid Pharmacotherapy Statistics Annual Data (NOPSAD) collection: provides information about people receiving opioid pharmacotherapy for their opioid dependence in Australia, as well as health professionals who prescribe opioid pharmacotherapy and dosing points (such as pharmacies) where clients receive treatment.
Agencies whose sole function is to prescribe or provide dosing services for opioid pharmacotherapy are excluded from the AODTS NMDS, as data from these agencies are captured in the NOPSAD collection (AIHW 2023a, 2023b).
Who uses alcohol and other drug treatment services?
Data from the AODTS NMDS indicate that around 131,000 clients aged 10 and over received AOD treatment in 2021–22. These clients received just over 228,000 closed treatment episodes (see glossary) from 1,274 publicly funded AOD treatment agencies.
In 2021–22:
- 6 in 10 clients of AOD treatment services were male (60% of clients), and around 5 in 10 were aged 20–39 years (52% of clients).
- Just under 2 in 10 clients (18%) identified as being an Aboriginal and/or Torres Strait Islander person.
- Over 9 in 10 clients sought treatment for their own drug use (93% of clients).
Between 2013–14 and 2020–21, the estimated number of clients receiving AOD treatment rose by 22%, before decreasing by 6% between 2020–21 and 2021–22. The rate of clients accessing AOD services increased from 564 to 619 clients per 100,000 population between 2013–14 and 2020–21, before decreasing to 576 clients per 100,000 in 2021–22.
The decrease in the estimated number of clients between 2020–21 and 2021–22, could be attributed to:
- client ability to access AOD services during public health restrictions
- impacts on the workforce with service staff becoming either unwell with COVID–19 or restrictions because of others’ COVID–19 status
- changes in funding for AOD services.
Who receives opioid pharmacotherapy treatment?
Data from the NOPSAD collection showed that around 55,700 clients received opioid pharmacotherapy treatment across Australia on a snapshot day in mid–2022. There were just under 3,200 dosing point sites nationally.
Opioid pharmacotherapy clients had broadly similar characteristics to clients of publicly funded AOD treatment agencies, but there was a higher proportion of people in older age groups. On a snapshot day in 2022:
- Almost 7 in 10 opioid pharmacotherapy clients were male (67% of clients), and nearly 6 in 10 were aged 30–49 (58% of clients).
- Just over 1 in 10 clients (12%) identified as being an Aboriginal and/or Torres Strait Islander person.
Between 2013–2022, the number of clients receiving opioid pharmacotherapy treatment increased by 17%. Across the same period, after adjusting for population growth, the rate of clients accessing opioid pharmacotherapy treatment has remained consistent at 21 clients per 10,000 population.
What drugs do people seek treatment for?
Data from the AODTS NMDS indicate that alcohol continued to be the most common principal drug of concern (PDOC) (see glossary) that led clients to seek treatment for their own drug use in 2021–22.
Between 2012–13 and 2021–22:
- The proportion of closed treatment episodes provided for alcohol as a PDOC decreased from 41% in 2012–13 to 32% in 2015–16 before increasing to 42% in 2021–22 (in relation to all principal drugs of concern).
- The second most common PDOC in 2021–22 was amphetamines. The proportion of closed treatment episodes for amphetamines rose from 14% in 2012–13 to 24% in 2021–22 (Figure 1).
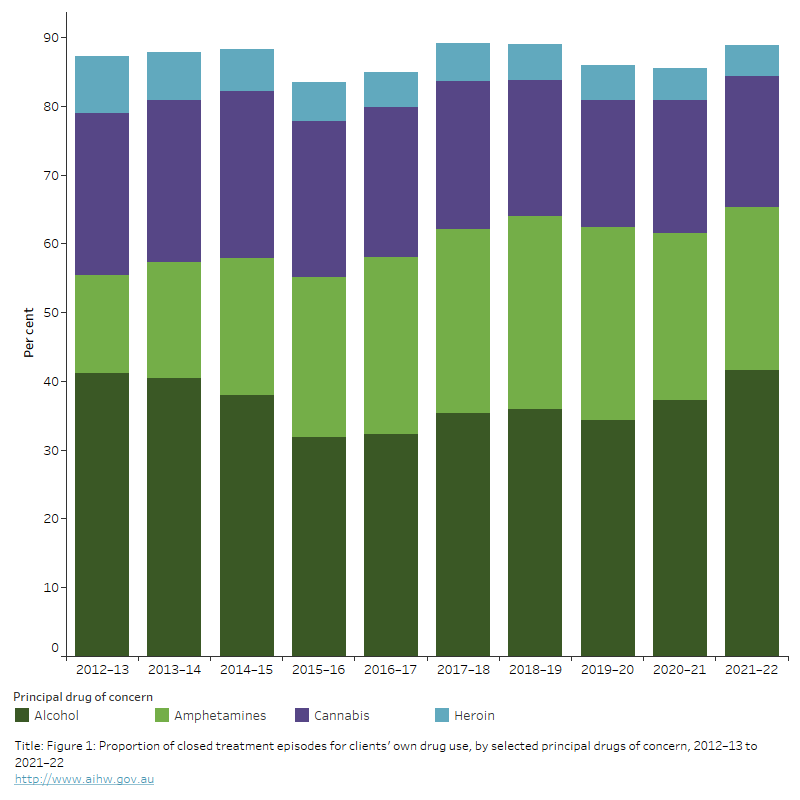
Figure 1: Proportion of closed treatment episodes for clients’ own drug use, by selected principal drugs of concern, 2012–13 to 2021–22
Figure 1: Proportion of closed treatment episodes for clients’ own drug use, by selected principal drugs of concern, 2012–13 to 2021–22
The stacked bar graph shows that from 2012–13 to 2021–22. Alcohol, amphetamines, cannabis, and heroin have remained the 4 most common principal drugs of concern across the period.
In 2021–22, 42% of closed treatment episodes were for alcohol as the principal drug of concern, 24% were for amphetamines, 19% were for cannabis and 4.5% were for heroin.
Notes
- In July 2021, WA decommissioned the central client management system that organisations used to record AODTS NMDS data which has potentially impacted WA AODTS NMDS data published in 2020–21.
- SA reports a high proportion of treatment episodes where amphetamines are the principal drug of concern due to the SA Police Drug Diversion Initiative (PDDI). In addition, adult cannabis offences are not included in the PDDI due to the SA Cannabis Expiation Notice legislation.
- Victoria reported relatively high incidences of ‘All other drugs’ due to service provider reporting practices and limitations with the data reporting system. This system was replaced in 2019–20. In 2019–20 and 2020–21, Victoria continued to report high levels of miscellaneous episodes coded as ‘Other drugs’ or ‘Not stated’ as principal drugs of concern due to service provider reporting practices with the new data reporting system.
- In Queensland, the level of cannabis reported as the principal drug of concern is a result of the police and illicit drug court diversion programs operating in the state.
- The AODTS NMDS also collects data on a client's additional drugs of concern, but this variable is not included in these data visualisations.
- Data are subject to minor revisions over time.
- Components of tables may not sum to totals due to rounding.
Source: AIHW 2023a.
AODTS NMDS data indicate that there is variation across age groups in terms of the most common PDOC. In 2021–22:
- Cannabis was the most common PDOC for young people, accounting for 61% of closed treatment episodes provided to clients aged 10–19 and 31% to clients aged 20–29.
- Amphetamines was the most common PDOC for people aged 20–29 (25% of treatment episodes) and 30–39 (33%).
- Alcohol was the most common PDOC for older people, accounting for 36% of treatment episodes provided to clients aged 30–39, 49% of episodes for those aged 40–49, 64% of episodes for those aged 50–59, and 77% of episodes for those aged 60 and over.
Data from the NOPSAD collection showed that heroin remained the most common opioid drug of dependence among opioid pharmacotherapy clients in 2022 (36%). Consistent with previous years, there was a high proportion of clients with ‘Not stated/not reported’ as the opioid drug of dependence (38% of clients) (Figure 2).
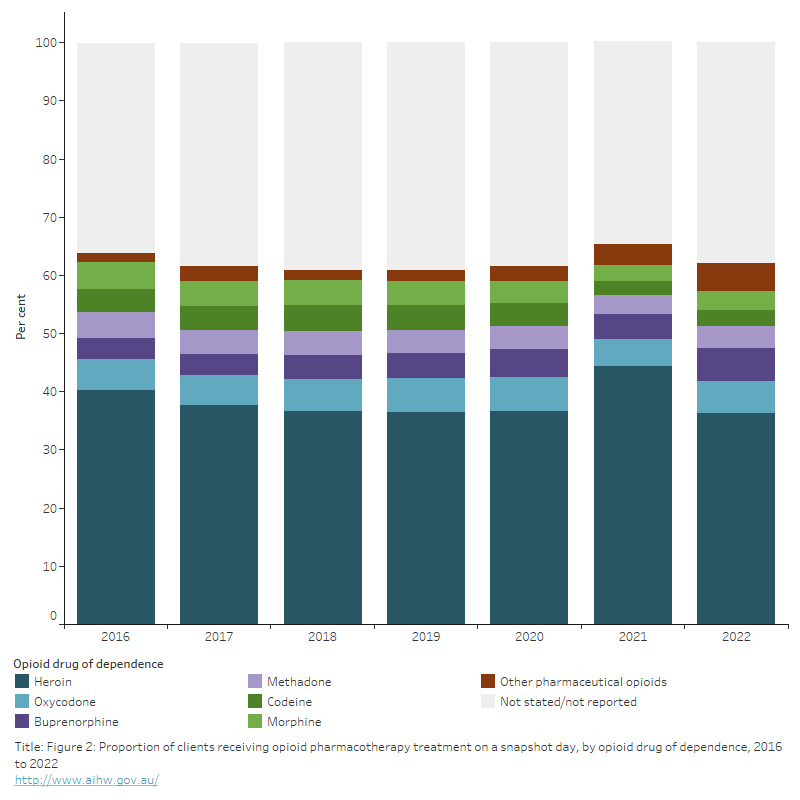
Figure 2: Proportion of clients receiving opioid pharmacotherapy treatment on a snapshot day, by opioid drug of dependence, 2016 to 2022
Figure 2: Proportion of clients receiving opioid pharmacotherapy treatment on a snapshot day, by opioid drug of dependence, 2016 to 2022
The stacked bar graph shows that between 2016 and 2022, heroin was the most common opioid drug of dependence among pharmacotherapy clients (excluding ‘Not stated/not reported’). In 2022, 36% of clients reported heroin as their drug of dependence. Across the period, there was a high proportion of Not stated/not reported responses (38% in 2022).
Notes
- 'Not stated/not reported' also includes 'Inadequately described' responses.
- NSW counts 'buprenorphine-naloxone' and 'buprenorphine LAI' as 'buprenorphine'.
- In 2020 and 2021, the increase in NSW client numbers could be attributed to the introduction of buprenorphine LAI (reported in the NOPSAD collection for the first time in 2020). Additional prescribing of buprenorphine occurred in correctional facilities, with the introduction of depot buprenorphine LAI during the year contributing to an increase in access to treatment. Some NSW Local Health Districts also reported having capacity to increase the number of new patients due to buprenorphine LAI.
- In 2020, the increase in Vic clients numbers may have been influenced by the implementation of the Victorian Governments SafeScript initiative. SafeScript has identified people with risky prescription opioid use who were previously undetected.
- In 2021, changes to coding practices in Vic may have led to a decreased number of clients with 'Not stated/not reported' as the drug of dependence, and corresponding increases for some other drug categories (for example, heroin).
- In 2021, data for Qld were not available. Total excludes Qld.
Source: AIHW 2023b.
What types of treatment do people receive?
Data from the AODTS NMDS indicate that counselling continues to be the most common main treatment type for clients accessing AOD treatment. Among clients seeking support for their own alcohol or drug use, 37% of treatment episodes in 2021–22 involved counselling as a main treatment and 22% involved an assessment only (Figure 3).
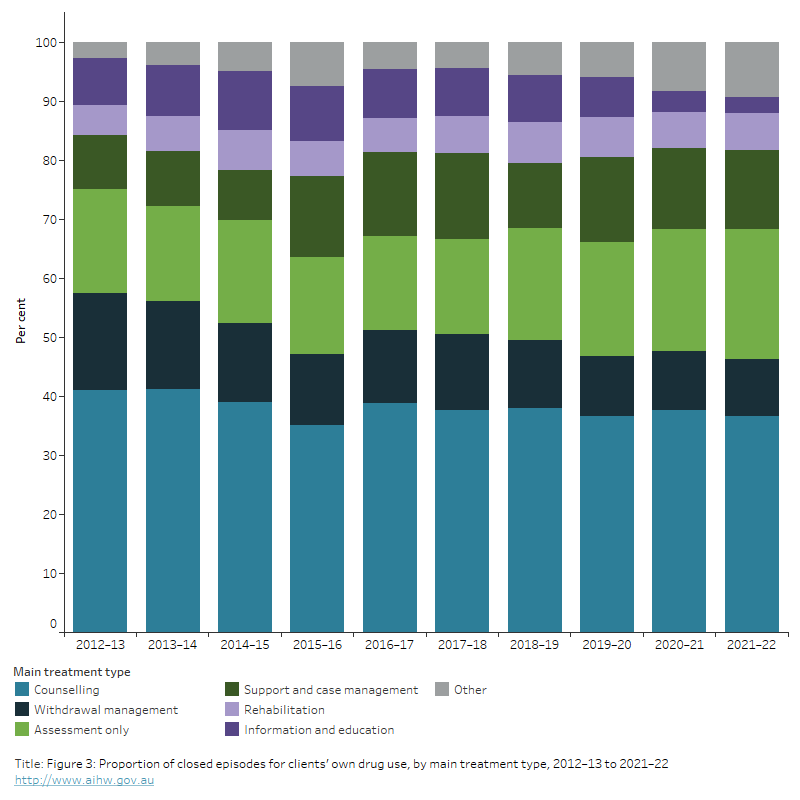
Figure 3: Proportion of closed episodes for clients’ own drug use, by main treatment type, 2012–13 to 2021–22
Figure 3: Proportion of closed episodes for clients’ own drug use, by main treatment type, 2012–13 to 2021–22
The stacked bar graph shows the closed treatment episodes for clients’ own drug use by main treatment type, from 2012–13 to 2021–22. In 2021–22, counselling was the most common main treatment type (37% of closed treatment episodes), followed by assessment only (22%) and support and case management (13%).
Notes
- In July 2021, WA decommissioned the central client management system that organisations used to record AODTS NMDS data which has potentially impacted WA AODTS NMDS data published in 2020–21.
- 'Other' includes pharmacotherapy.
- Rehabilitation, withdrawal management (detoxification), and pharmacotherapy are not available for clients seeking treatment for someone else’s alcohol or other drug use.
- In 2019–20, changes were made to categories under Main Treatment; the word ‘only’ was removed from support and case management and information and education. The removal of the word ‘only’ from support and case management and information and education, changed reporting rules for agencies; allowing agencies to be able to report and more accurately capture these items as an additional treatment in conjunction with a main treatment type.
- The AODTS NMDS also collects data on a client's other treatment types, as well as main treatment type, however, this variable is not included in these data visualisations.
- SA reports a high proportion of Assessment only treatment episodes due to legislated client assessments under the state’s Police Drug Diversion Initiative and child protection programs.
- Data are subject to minor revisions over time.
- Components of tables may not sum to totals due to rounding.
Source: AIHW 2023a.
Data from the NOPSAD collection showed that methadone continues to be the most common pharmacotherapy drug provided to opioid pharmacotherapy clients. On a snapshot day in 2022, 50% of opioid pharmacotherapy clients received methadone as pharmacotherapy treatment, and 46% of clients received a buprenorphine opioid drug formulation (see glossary). Over the past decade, the proportion of clients receiving methadone has fallen from 68% in 2013 to 50% in 2022. Conversely, the proportion of clients receiving a buprenorphine opioid drug formulation has increased from 33% in 2013 to 46% in 2022, in part reflecting the availability of new buprenorphine opioid drug formulations such as buprenorphine long-acting injection (LAI).
How has COVID-19 impacted alcohol and other drug treatment services ?
Measures put in place to reduce the transmission of COVID–19 introduced new challenges for clinicians and clients accessing AOD treatment services and opioid pharmacotherapy. These challenges included:
- regulatory changes to support treatment delivery
- maintaining effective social distancing measures, particularly where people are required to visit an opioid dosing site daily or where specialist AOD treatment is in bed-based health settings.
Impact of COVID-19 on alcohol and other drug treatment services
In response to COVID-19 restrictions, AOD treatment service providers across all jurisdictions have made changes to modes of treatment delivery. The aim was to support flexible treatment delivery and maintain the health and safety of clients and treatment service providers. While these changes varied across jurisdictions, changes included:
- decreased bed capacity at residential rehabilitation and withdrawal services, or closure of these services for a period of time
- ceased or reduced intake of new clients to residential rehabilitation and withdrawal services
- adoption of telehealth including using phone, online and video conferencing (to deliver services in the place of face-to-face contact)
- group sessions were cancelled, or moved to telehealth forums
- prescription review periods increased
- increased wait-time periods between referrals and admissions to AOD treatment due to reduced capacity.
Impact of COVID-19 on opioid pharmacotherapy
In response to COVID–19 restrictions, states and territories made temporary changes to opioid pharmacotherapy treatment guidelines and regulations. The aim was to support flexible treatment delivery and maintain the health and safety of patients and prescribers. While the implementation of these amended guidelines and regulations vary across jurisdictions, changes to pharmacotherapy treatment in the context of COVID–19 have included:
- extending prescription duration
- increasing the number of takeaway doses and arranging home delivery of medication
- considering changing clients to buprenorphine LAI wherever appropriate
- a transition to online delivery modes for pharmacist training and education on administering opioid pharmacotherapy treatment
- the commencement of buprenorphine LAI under online supervision (with dosing administered in person at a pharmacy).
Where do I go for more information?
For more information on alcohol and other drug treatment services and opioid pharmacotherapy in Australia, see:
- Alcohol and other drug treatment services in Australia: early insights
- National Opioid Pharmacotherapy Statistics Annual Data collection
- Alcohol, tobacco & other drugs in Australia
Visit Alcohol & other drug treatment services for more on this topic.
AIHW (Australian Institute of Health and Welfare) (2022) Alcohol, tobacco & other drugs in Australia, AIHW, Australian Government, accessed 14 April 2023.
AIHW (2023a) Alcohol and other drug treatment services in Australia: Early insights, AIHW, Australian Government, accessed 14 April 2023.
AIHW (2023b) National Opioid Pharmacotherapy Statistics Annual Data collection, AIHW, Australian Government, accessed 20 April 2023.
Department of Health and Aged Care (2019) National Framework for Alcohol, Tobacco and Other Drug Treatment 2019–29, Department of Health and Aged Care, Australian government, accessed 1 March 2023.


