Length of stay overview
Median length of stay and the effect of specific conditions are reported for people living with dementia and people without dementia by their change in usual residence or mortality within 7-days of discharge from hospital.
First Hospitalisation
For people aged 65 or older, this study reports on the characteristics of each person’s first hospitalisation ending in 2017 and their transitions of care before and after. This includes hospital admissions that started in 2017 (or earlier) that resulted in discharge or death in 2017. For people who had more than one hospitalisation ending in 2017, the first hospitalisation is the one that occurred earliest in the year.
People who lived in the community prior to first hospitalisation
Nearly 2 in 3 people living with dementia (62%) and 97% of people without dementia lived in the community prior to their first hospitalisation (Figure 13 and Table S1.5).
Within 7-days of discharge from their first hospitalisation:
- 71% of people living with dementia and 95% of people without dementia returned to live in the community (community-dwellers)
- 23% of people living with dementia and 2% of people without dementia transitioned to residential aged care
- 5% of people living with dementia and 3% of people without dementia died (during hospitalisation or within 7-days after discharge).
People who lived in residential aged care prior to first hospitalisation
Over 1 in 3 people living with dementia (38%) and 3% of people without dementia lived in residential aged care prior to their first hospitalisation. Within 7-days of discharge from their first hospitalisation:
- 86% of people living with dementia and 89% of people without dementia returned to live in residential aged care (aged care residents)
- 14% of people living with dementia and 11% of people without dementia died (during hospitalisation or within 7-days after discharge).
Figure 13 Change in usual residence or mortality within 7-days of discharge for people living with dementia and people without dementia
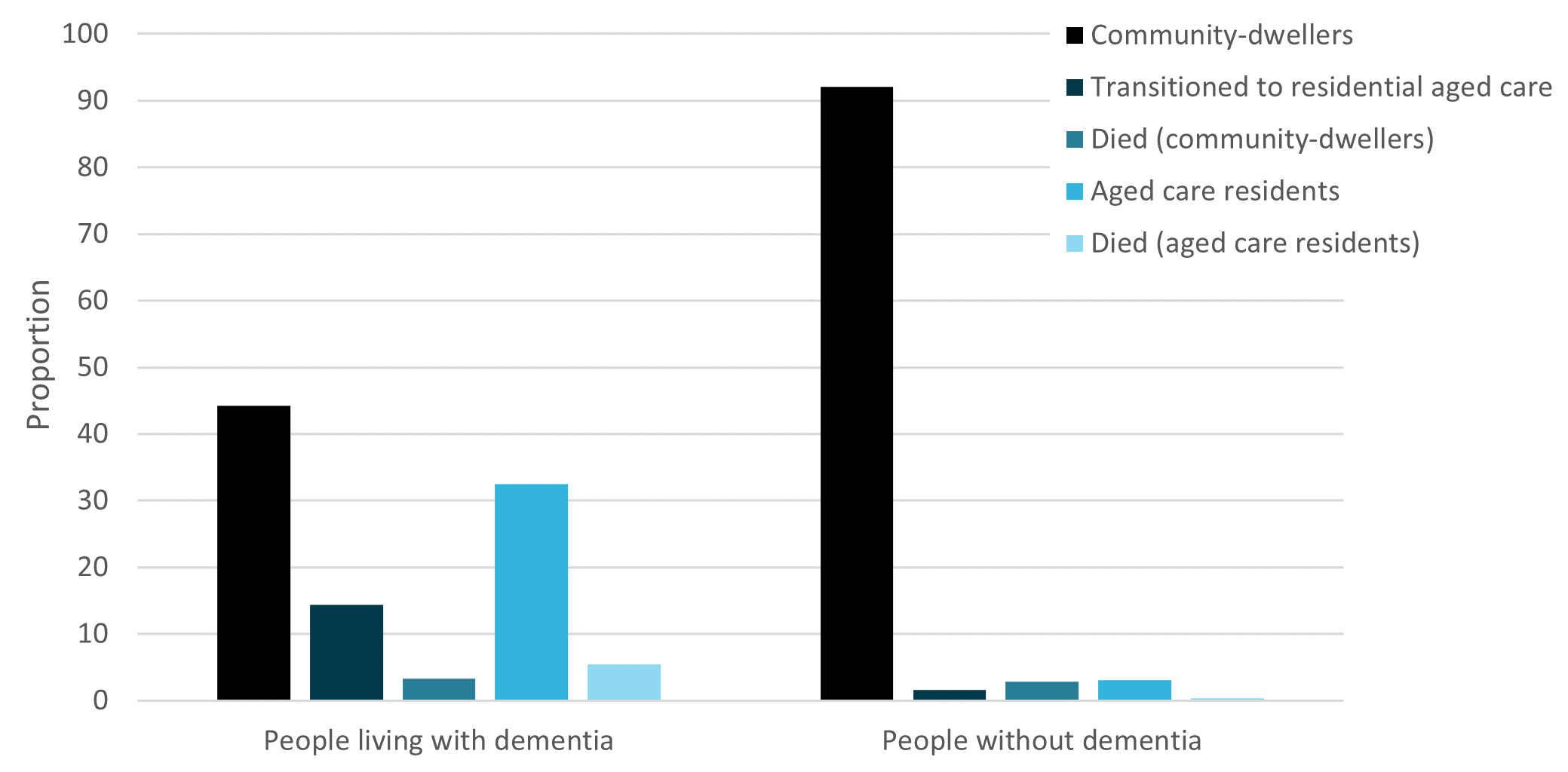
Source: AIHW NIHSI 2018–19, analysis of NIHSI.


