Communicable diseases
Communicable diseases, or infectious diseases, are spread from one person to another, or from an animal to a person, through viruses or bacteria in the air, food, blood or other bodily fluids. The Australian Government monitors communicable diseases through the National Notifiable Diseases Surveillance System, which coordinates the surveillance of more than 50 communicable diseases (Department of Health 2016).
Due to good sanitation practices, and the use of antibiotics and immunisation programs, communicable diseases are not generally a major issue in Australia (AIHW 2022). But, some communicable diseases – particularly bloodborne viruses, and sexually transmissible infections (STIs) – are more prevalent in the prison population than in the wider Australian community (Butler and Simpson 2017).
This is due, in part, to the higher level of at-risk behaviours that people engage in before and during incarceration, compared with the general population. These include injecting drug use, needle-sharing, unsafe sexual practices, amateur tattooing and physical violence (Butler and Simpson 2017).
COVID-19 outbreaks have been reported in prisons across Australia. Given the high level of vulnerability of the prison population, COVID-19 poses a serious risk to the physical health of prisoners. Measures introduced to reduce the spread of COVID-19 are also likely to have had an impact on the mental, emotional and social wellbeing of people in prison (Department of Health 2020).
Prison entrants who received a COVID-19 vaccine
In 2022, almost 4 in 5 (79%) prison entrants reported receiving a COVID-19 vaccine; of those entrants, almost 1 in 2 (47%) reported they had received 3 doses. The proportion of prison entrants who had reported receiving a COVID-19 vaccine ranged from 73% of those aged 25–34 to 85% of those aged 35–44.
Male entrants (79%) and female entrants (78%) were similarly as likely to report they had received a COVID-19 vaccine. Male entrants (48%) were more likely than female entrants (38%) to report they had received 3 doses of the COVID-19 vaccine (Figure 3.3).
First Nations entrants (85%) were more likely to report receiving a COVID-19 vaccine than non-Indigenous entrants (75%). Of First Nations entrants that reported receiving a COVID-19 vaccine, a half (50%) stated that they had received 3 doses (Figure 3.3).
Figure 3.3: Prison entrants, self-reported number of COVID-19 vaccine doses received, 2022
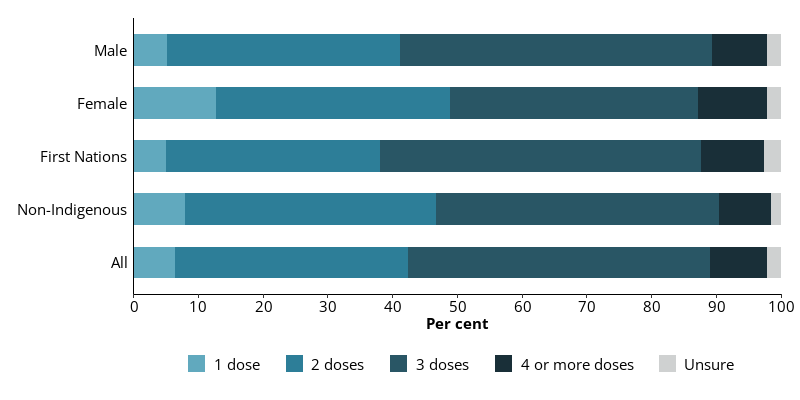
Notes
- Proportions are representative of this data collection only, and not the entire prison population.
- Proportions are representative of 294 prison entrants who reported being vaccinated against COVID-19 only.
- Excludes Victoria, which did not provide data for this item.
Source: Entrants form, 2022 NPHDC.
Prison dischargees experiences with COVID-19
In 2022, more than 4 in 5 (84%) dischargees reported being quarantined or isolated due to COVID-19 while in prison. Dischargees aged 18–24 (71%) were least likely to report being quarantined or isolated due to COVID-19 while in prison. Male dischargees (83%) and female dischargees (84%) were similarly as likely to report having been quarantined or isolated due to COVID-19 while in prison.
Almost 9 in 10 (85%) prison dischargees reported being offered a COVID-19 vaccine while in prison. Of those dischargees, almost 7 in 10 (69%) reported receiving the COVID-19 vaccine while in prison.
Dischargees aged 18–24 (90%) were most likely to report being offered the COVID-19 vaccine while in prison, and dischargees aged 25–34 (82%) were least likely.
Male dischargees (86%) were more likely to report being offered the COVID-19 vaccine while in prison than female dischargees (80%).
Almost three-quarters (73%) of First Nations dischargees and two-thirds (65%) of non‑Indigenous dischargees reported receiving a COVID-19 vaccine while in prison.
STIs are a continuing public health concern in Australia (Department of Health 2018), particularly for some groups of people, including those in prison.
The incidence of some STIs, such as human papillomavirus, has declined drastically in recent years, mostly due to the introduction of a human papillomavirus vaccine. But, other STIs – such as chlamydia, gonorrhoea and syphilis – have increased (Department of Health 2019).
The Australian Government monitors the prevalence of certain STIs through the National Notifiable Diseases Surveillance System. Notifiable STIs include chlamydial infection, donovanosis, gonococcal infection, and syphilis (Department of Health 2018).
In 2021, there were 121,793 notifications of STIs in Australia (Department of Health and Aged Care 2023b). The NPHDC collected data from jurisdictions on the number of notifications of STIs in prisons for these infections during the 2021 calendar year.
During 2021, there were 18,650 notifications of STIs for people in custody in New South Wales, Queensland, Western Australia, South Australia, Tasmania and the Northern Territory (Indicator 1.2.2).
The rate of notifications of STIs for prisoners received into custody in 2021 was 53 per 100 prisoners received into custody.
The hepatitis C virus is an infection that causes liver inflammation; if left untreated, it can lead to complications such as cirrhosis (a chronic liver disease) and cancer (Wallace et al. 2018). It is the most commonly reported notifiable bloodborne disease in Australia (Department of Health and Aged Care 2023a).
The prison population is especially at risk of hepatitis C infection, due to the high proportion of people in custody with a history of injecting drug use; the at-risk behaviours associated with illicit and injecting drug use, including needle-sharing; and other at-risk behaviours, such as amateur tattooing and violence that can lead to blood-to-blood contact (Department of Health and Aged Care 2023c).
People in prison often come from marginalised groups, where medical care in the community is unavailable or not accessed, so are at risk of having undiagnosed hepatitis C before entering prison (Department of Health and Aged Care 2023c; Wallace et al. 2018).
Prison clinics are an ideal place to detect and treat people with undiagnosed hepatitis C. In recent years, new medications for the disease have led to an enormous increase in the treatment rate of people in prison with hepatitis C (Department of Health and Aged Care 2023c). For information on hepatitis C medication dispensed in prisons, see Medications.
In the past, the NPHDC has reported on the proportion of prison entrants testing positive to hepatitis C using the National Prison Entrants’ Bloodborne Virus & Risk Behaviour Survey. This survey has now been replaced by AusHep; however, AusHep data were not available when writing this report.
Hepatitis C surveillance
As part of the NPHDC, jurisdictions were asked to provide the number of tests performed for hepatitis C (antibody tests, polymerase chain reaction [PCR] tests and genotype tests) during the calendar year. Data on positive test results were not requested; however, the number of tests performed provides some surveillance data.
During 2021, there were 37,181 tests performed for hepatitis C for people in custody in New South Wales, Queensland, Western Australia, South Australia and the Northern Territory (Indicator 1.2.3).
Hepatitis C testing for prison dischargees
In 2022, prison dischargees were asked whether they had received a test for hepatitis C in prison and, if so, the test result.
Almost 2 in 3 (64%) prison dischargees reported that they had been tested for hepatitis C in prison (Indicator 1.2.4).
One in 13 (8.1%) dischargees tested positive for hepatitis C in prison, while almost half (45%) tested negative. About one-third (32%) of dischargees were not tested for hepatitis C in prison.
Hepatitis B is a bloodborne virus that causes inflammation of the liver, and can lead to cirrhosis and cancer, conditions that can be fatal (Department of Health and Aged Care 2023b).
In 2020, over 220,000 people in Australia were living with a chronic hepatitis B infection. A vaccination for hepatitis B has been available since the 1980s, but the virus still disproportionately affects many disadvantaged populations, including people born overseas, First Nations peoples, and people in custody (Department of Health and Aged Care 2023b).
As part of the NPHDC, jurisdictions were asked to provide the number of tests performed for hepatitis B during the calendar year. Data on positive test results were not requested; however, the number of tests performed provides some surveillance data.
During 2021, there were 79,756 tests performed for hepatitis B for people in custody in New South Wales, Queensland, Western Australia, South Australia, and the Northern Territory (Indicator 1.2.5).
Human immunodeficiency virus (HIV) is a bloodborne virus that weakens the immune system; if left untreated, it can eventually lead to acquired immunodeficiency syndrome (AIDS). While there is no effective cure available for HIV, treatment in the form of medication can prevent disease progression and transmission (Department of Health 2019).
Although prevalence is low in the prison population, transmission remains a risk due to higher levels of at-risk behaviours that people engage in (Butler and Simpson 2017).
As part of the NPHDC, jurisdictions were asked to provide the number of tests performed for HIV during the calendar year. Data on positive test results were not requested; however, the number of tests performed provides some surveillance data.
During 2021, there were 57,527 tests performed for HIV for people in custody in New South Wales, Queensland, Western Australia, South Australia, and the Northern Territory (Indicator 1.2.6).
(2022) Infectious and communicable diseases, AIHW, Australian Government, accessed 03 October 2023.
Butler T and Simpson M (2017) National Prison Entrants’ Bloodborne Virus and Risk Behaviour Survey 2004, 2007, 2010, 2013 and 2016, Kirby Institute, University of New South Wales, Sydney.
Department of Health (2016) ‘Surveillance systems reported in Communicable Diseases Intelligence, 2016’, Communicable Diseases Intelligence 40(1):E11–E16.
—— (2018) Fourth National Sexually Transmissible Infections Strategy 2018–2022, Department of Health, Australian Government, accessed 17 April 2023.
—— (2019) Eighth National HIV Strategy 2018–2022, Department of Health, Australian Government, accessed 8 June 2023.
—— (2020) CDNA National Guidelines for COVID-19 Outbreaks in Correctional and Detention Facilities, Department of Health, Australian Government, accessed 29 September 2023.
Department of Health and Aged Care (2023a) Fourth National Hepatitis B Strategy
2023–2030, Department of Health and Aged Care, Australian Government, accessed 8 June 2023.
—— (2023b) National Notifiable Diseases Surveillance System, Department of Health and Aged Care, Australian Government, accessed 3 May 2023.
—— (2023c) Sixth National Hepatitis C Strategy 2023–2030, Department of Health and Aged Care, Australian Government, accessed 15 August 2023.
Wallace J, Richmond J, Ellard J, Power J and Lucke J (2018) ‘Eradicating hepatitis C: the need for a public health response’, Global Public Health, 13(9):1254–64.


